Definisi
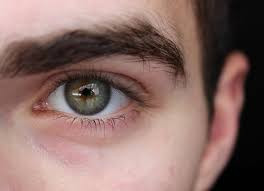
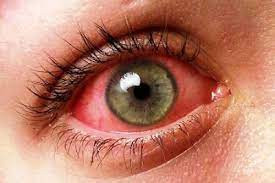
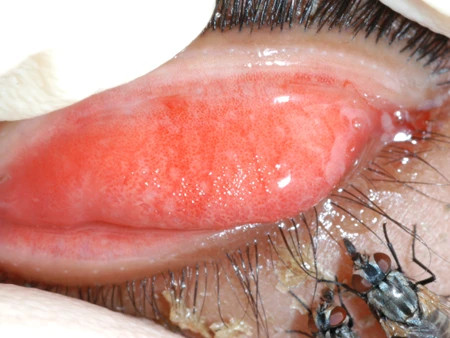
Uveitis adalah peradangan yang terjadi pada lapisan tengah mata yang disebut dengan uvea. Uvea adalah lapisan tengah mata yang terdiri atas selaput pelangi mata (iris), lapisan pembuluh darah mata (koroid), dan jaringan ikat antara iris dan koroid (badan siliar). Uvea terletak di antara bagian putih mata dan bagian belakang mata yang menangkap cahaya. Uvea sangat penting karena mengandung banyak pembuluh darah yang mengantarkan darah ke bagian lain mata. Apabila terjadi radang pada bagian ini, maka dapat ditandai dengan mata yang terlihat sangat merah, nyeri, dan penglihatan kabur.
Penyakit ini lebih banyak terjadi pada usia 20-50 tahun. Uveitis dapat memengaruhi kualitas penglihatan karena beberapa kasus dapat bersifat kronis dan mengakibatkan penyakit lain. Penyakit-penyakit lainnya yaitu katarak, glaukoma, serta risiko kebutaan permanen. Sekitar 10% dari kasus kebutaan berawal dari adanya uveitis.
Uveitis dapat dibagi menjadi beberapa tipe berdasarkan lokasi peradangannya, yaitu uveitis di area bagian depan (iris), uveitis di bagian tengah (antara iris dan koroid), uveitis di bagian belakang (koroid), serta uveitis di seluruh area atau yang biasa disebut panuveitis (terjadi pada seluruh bagian uvea). Selain itu, uveitis juga dapat bersifat akut apabila gejala membaik dalam kurun waktu kurang dari 3 bulan dan bersifat kronik apabila terjadi lebih dari 3 bulan.
Penyebab
Kurang lebih 50% kasus uveitis terjadi akibat penyebab yang tidak diketahui, bahkan orang sehat juga dapat tiba-tiba mengalami uveitis. Namun, sebagian besar kasus nya juga berkaitan dengan gangguan sistem daya tahan tubuh seseorang terutama bila seseorang mengalami penyakit autoimun. Beberapa penyakit autoimun yang dikaitkan sebagai pemicu uveitis adalah sebagai berikut:
- Psoriasis, jenis penyakit autoimun yang menyebabkan peradangan pada kulit.
- Artritis reumatoid, yaitu penyakit autoimun yang menyebabkan peradangan pada sendi.
- Ankylosing spondylitis, yaitu penyakit autoimun yang menyebabkan radang sendi pada tulang belakang.
- Sarkoidosis, yaitu penyakit autoimun yang menyebabkan radang yang muncul di berbagai bagian tubuh seperti paru, kelenjar getah bening, mata, dan kulit.
- Penyakit kawasaki, yaitu penyakit autoimun yang menyebabkan radang pada dinding pembuluh darah.
- Kolitis ulseratif, yaitu penyakit autoimun yang menyebabkan radang usus besar.
- Penyakit Crohn, yaitu penyakit autoimun yang menyebabkan radang pada saluran pencernaan.
Selain penyakit autoimun, beberapa kasus uveitis juga diduga akibat adanya infeksi, misalnya virus varisela zoster, herpes, tuberkulosis, sifilis, dan sebagainya. Penyebab di luar infeksi pun juga dapat menjadi pemicu terjadinya uveitis. Misalnya, adanya cedera atau riwayat operasi mata, keganasan atau kanker pada mata, serta pajanan racun pada mata.
Faktor Risiko
Diketahui bahwa orang yang memiliki genetik tertentu dapat lebih rentan terkena uveitis. Begitu pula dengan orang yang memiliki penyakit autoimun dan adanya riwayat operasi mata. Meski demikian, penyebab pasti dari uveitis kadang tidak diketahui.
Kebiasaan merokok dan usia lebih dari 60 tahun juga dapat meningkatkan risiko terjadinya uveitis yang lebih berat. Selain itu, faktor usia juga berperan dalam meningkatkan risiko terjadinya komplikasi uveitis.
Gejala
Uveitis dapat muncul secara tiba-tiba atau berkembang secara bertahap. Gejala-gejala yang dapat muncul antara lain:
- Mata merah
- Mata terasa nyeri
- Penglihatan kabur
- Sensitif terhadap cahaya
- Muncul bintik hitam atau floaters dalam pandangan mata
- Penurunan tajam penglihatan
Diagnosis
Dokter akan memeriksa riwayat kesehatan dan gejala yang dirasakan, setelah itu diperlukan pemeriksaan fisik pada mata untuk menegakkan diagnosis. Pemeriksaan penunjang hanya dilakukan untuk mendapatkan hasil diagnosis yang lebih akurat. Pemeriksaan penunjang tidak diperlukan pada kondisi uveitis akut yang memiliki gejala ringan/sedang tanpa ada penyakit penyerta atau kondisi yang sudah dapat dipastikan melalui pemeriksaan gejala dan fisik, seperti Fuchs Uveitis Syndrome (FUS) atau sarkoidosis.
Pemeriksaan penunjang yang mungkin dilakukan, seperti:
- Pemeriksaan tajam penglihatan
- Pemeriksaan tekanan bola mata dengan tonometri
- Pemeriksaan struktur mata dengan slit lamp
- Pemeriksaan bagian dalam mata dengan funduskopi
- Pemeriksaan darah
- Serta pencitraan mata untuk mengukur ketebalan dan melihat adanya sel radang pada mata
Pemeriksaan penunjang seperti CT Scan atau MRI hanya diperlukan apabila terdapat indikasi atau ingin mencari penyebab penyakit lain yang mendasari uveitis.
Tata Laksana
Tujuan utama pengobatan uveitis adalah mengurangi peradangan pada mata. Tatalaksana uveitis dapat dilakukan dengan pemberian obat-obatan hingga prosedur operasi.
Beberapa jenis obat-obatan yang dapat direkomendasikan dokter sebagai tatalaksana uveitis adalah sebagai berikut:
- Kortikosteroid, obat-obatan ini dapat mengurangi peradangan.
- Antibiotik atau antivirus, obat-obatan ini diberikan sesuai dengan jenis infeksi yang menyebabkan uveitis. Obat-obatan ini perlu dikonsumsi secara rutin dan dihabiskan sesuai dengan resep dokter.
- Obat penekan daya tahan tubuh, diberikan bila uveitis terjadi pada kedua mata atau tidak berhasil ditangani dengan kortikosteroid. Namun, obat jenis ini juga memerlukan pengawasan yang ketat agar mengurangi efek samping yang dapat terjadi. Obat ini hanya dapat dikonsumsi sesuai dengan indikasi dan anjuran dokter.
Apabila gejala uveitis cukup parah dan tidak membaik dengan obat-obatan, maka dokter mungkin merekomendasikan beberapa prosedur operasi. Salah satunya adalah vitrektomi, yaitu operasi bedah mata untuk mengambil cairan dari bagian dalam mata atau disebut juga cairan vitreus. Prosedur operasi lain yang dapat direkomendasikan adalah operasi penanaman alat pelepas obat, yaitu ditanamnya alat khusus untuk menyalurkan obat jenis kortikosteroid secara perlahan ke dalam mata. Pengobatan dengan alat ini umumnya selama 2-3 tahun. Jenis pengobatan dan lamanya penanganan uveitis bergantung pada tingkat keparahan uveitis yang dialami.
Komplikasi
Uveitis yang tidak ditangani dengan tepat dapat menimbulkan beberapa komplikasi seperti:
- Katarak
- Glaukoma
- Ablasio retina, yaitu lepasnya retina dari lapisan pembuluh darah yang memberi nutrisi dan oksigen ke mata
- Pembengkakan pada retina mata
- Peradangan yang menyebabkan lapisan iris melekat pada lensa mata
Pencegahan
Secara umum, uveitis merupakan penyakit yang sulit dicegah. Hal ini dikarenakan sebagian besar kasus nya disebabkan karena faktor yang tidak diketahui. Namun, apabila kondisi ini dapat dideteksi dan diobati secara cepat dan tepat, maka dapat mengurangi komplikasi. Kemungkinan terburuk yang dapat dicegah adalah terjadinya kebutaan permanen.
Kapan Harus ke Dokter?
Apabila Anda merasakan gejala yang mengarah ke uveitis, sebaiknya segera memeriksakan diri ke dokter mata terdekat. Hal tersebut terutama bila Anda memiliki penyakit penyerta lainnya, seperti penyakit autoimun yang dapat menjadi pemicu terjadinya uveitis.
Mau tahu lebih lanjut seputar penyakit-penyakit lainnya? Cek di sini, ya!
- dr Ayu Munawaroh, MKK
- dr Hanifa Rahma
Mayo Clinic. Uveitis. Available from: https://www.mayoclinic.org/diseases-conditions/uveitis/symptoms-causes/syc-20378734.
NHS. Uveitis. Available from: https://www.nhs.uk/conditions/uveitis/.
Griff AM. Uveitis (2018). Available from: https://www.healthline.com/health/uveitis.
National Eye Institute. Uveitis. Available from: https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/uveitis.
The Ocular Immunology and Uveitis Foundation. Uveitis symptoms and causes. Available from: https://uveitis.org/.
American Academy of Ophthalmology. Uveitis. Available from: https://www.aao.org/eye-health/diseases/what-is-uveitis.
Bowling B. Kanski’s clinical ophthalmology. Edisi ke-8. Philadelphia:Elsevier;2016.