Definisi
Kusta (nama lain: penyakit Hansen, lepra) merupakan penyakit infeksi yang menyebabkan luka pada kulit dan kerusakan saraf pada lengan, tungkai, dan bagian tubuh lainnya. Penyakit ini ada di seluruh dunia. Saat ini, di seluruh dunia, terdapat sekitar 208.000 orang yang terinfeksi kusta. Penderita kusta paling banyak berada di Afrika dan Asia, dan terutama pada daerah dengan iklim tropis atau subtropis.
Penyebab
Kusta disebabkan oleh bakteri Mycobacterium leprae. Kusta memiliki nama lain penyakit Hansen, sesuai dengan nama ilmuwan yang menemukan bakteri tersebut pada tahun 1873. Bakteri ini membelah secara lambat sehingga penyakit ini biasanya baru muncul rata-rata setelah 5 tahun. Gejala penyakit ini dapat muncul setelah 1 tahun, namun dapat pula muncul setelah 20 tahun atau lebih.
Penyebaran penyakit ini belum diketahui secara pasti, namun diduga menular lewat droplet atau titik-titik air yang menyebar saat seseorang batuk atau bersin. Tidak hanya itu, kontak fisik jarak dekat dengan orang yang menderita kusta juga dapat menularkan kusta. Kontak fisik singkat seperti berjabat tangan, berpelukan, atau duduk di sebelah orang tersebut saat naik kendaraan umum atau makan tidak dapat menularkan kusta. Ibu dengan kusta tidak dapat menyebarkan infeksi kepada janin yang dikandungnya, karena bakteri ini tidak dapat berpindah melalui ari-ari. Selain itu, penyakit ini tidak ditularkan lewat hubungan intim.
Faktor Risiko
Faktor risiko kusta adalah sebagai berikut:
- Kontak erat. Kontak erat secara langsung dengan penderita kusta meningkatkan risiko seseorang terkena penyakit kusta
- Paparan terhadap armadillo. Di daerah selatan Amerika Serikat, bakteri Mycobacterium leprae ditemukan secara alami pada armadillo. Namun, belum diketahui secara pasti penularan bakteri ini dari armadillo ke manusia
- Usia. Semakin lanjut usia, semakin tinggi risiko seseorang tertular kusta. Beberapa penelitian menunjukkan puncak penularan pada usia 5-15 tahun (anak) dan pada usia di atas 30 tahun
- Pengaruh genetik. Gen memengaruhi respon kekebalan tubuh seseorang dalam menghadapi bakteri ini, terlepas dari jarak kontak
- Imunosupresi. Obat-obatan yang menekan sistem kekebalan tubuh atau penyakit pada sistem kekebalan tubuh sendiri dapat menyebabkan seseorang lebih mudah mengalami kusta. Kusta biasanya terjadi setelah menerima cangkok organ, kemoterapi, infeksi HIV/AIDS, serta konsumsi obat-obatan untuk gejala penyakit autoimun (sel kekebalan tubuh menyerang bagian tubuh sendiri)
Gejala
Gejala utama penyakit kusta adalah:
- Kelemahan otot
- Rasa baal atau mati rasa pada tangan, lengan, kaki, dan tungkai
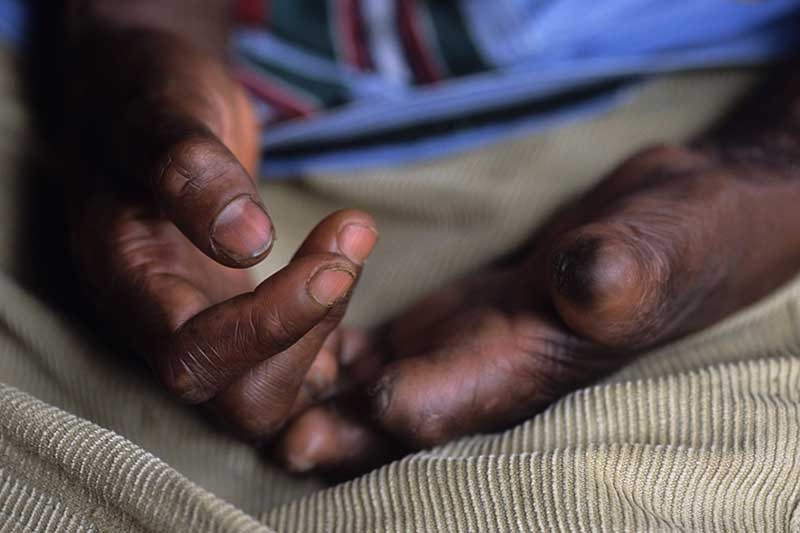
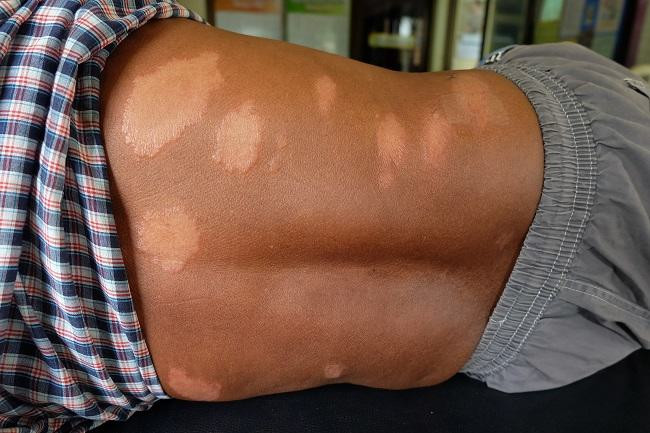
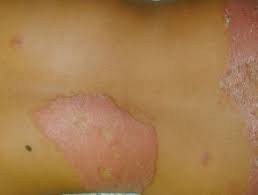
- Adanya penampakan luka pada kulit
- Luka pada kulit ini mengalami penurunan sensasi raba, suhu, dan nyeri. Gejala ini tidak hilang dalam beberapa minggu
- Biasanya, luka pada kulit ini tampak lebih terang daripada warna kulit alami atau merah karena peradangan
Untuk mendiagnosis penyakit kusta, dokter akan menghitung jumlah luka pada kulit dan saraf yang terpengaruh. Ilmu kedokteran saat ini mengenal tiga sistem klasifikasi kusta, yaitu tuberkuloid/lepromatosa, klasifikasi World Health Organization (WHO), dan klasifikasi Ridley-Jopling. Klasifikasi ini akan membedakan terapi kusta nantinya.
Klasifikasi tuberkuloid/lepromatosa tergantung pada respon kekebalan tubuh seseorang, yang dapat dijelaskan sebagai berikut:
- Kusta Tuberkuloid. Pada tipe ini, respon kekebalan tubuh baik, sehingga penyakit bergejala ringan dan tidak terlalu menular. Jumlah luka pada kulit pun lebih sedikit
- Kusta Lepramatosa. Pada tipe ini, respon kekebalan tubuh jelek, sehingga penyakit bergejala lebih berat dan sangat menular. Penyakit ini menyerang kulit, saraf, dan organ lainnya. Luka pada kulit pun berjumlah banyak dan dapat membentuk benjolan
- Kusta Borderline. Pada tipe ini, terdapat ciri dari tipe tuberkuloid dan lepromatosa sekaligus. Tipe ini berada di antara dua tipe sebelumnya
Sementara itu, klasifikasi World Health Organization (WHO) lebih sederhana, yaitu:
- Pausibasiler. Pada tipe ini, jumlah luka di kulit berjumlah kurang dari sama dengan lima, dan tidak ada bakteri terdeteksi pada pemeriksaan kerok kulit
- Multibasiler. Pada tipe ini, luka pada kulit berjumlah lebih dari lima atau bakteri tidak terdeteksi pada pemeriksaan kerok kulit
Klasifikasi Ridley-Jopling membagi penyakit ini menjadi lima berdasarkan keparahan gejala. Biasanya, klasifikasi ini digunakan untuk studi klinis.
Orang yang menderita kusta juga dapat mengalami reaksi kekebalan tubuh pada sebelum, saat, dan sesudah menjalani pengobatan. Terdapat dua reaksi kusta, yaitu tipe 1 (reaksi reversal) dan tipe 2 (eritema nodosum leprosum, ENL). Pada reaksi tipe 1, pasien dapat mengalami beberapa gejala berikut selama beberapa bulan:
- Kemerahan dan bengkak pada kulit dengan saraf besar atau wajah
- Kemerahan pada luka di kulit yang sudah ada
- Peradangan akibat reaksi yang menyebabkan perubahan bentuk kulit dan kelumpuhan
- Luka terbuka pada kulit
- Fungsi saraf melemah atau hilang
Sementara itu, reaksi tipe 2 (eritema nodosum leprosum), sesuai namanya, memiliki gejala berupa benjolan kemerahan yang tiba-tiba muncul dan terasa nyeri. Benjolan ini dapat mendekati permukaan kulit atau terletak dalam. Biasanya, benjolan ini muncul pada anggota gerak tubuh dan hilang dalam beberapa hari.
Diagnosis
Jika Anda dicurigai menderita kusta, dokter akan melakukan pemeriksaan saraf pada bagian kulit tersebut. Jika bagian kulit tersebut mati rasa, dokter dapat memutuskan untuk melanjutkan pemeriksaan dengan kerok kulit. Luka pada kulit tersebut akan dikerok sedikit dan diperiksa di laboratorium. Pemeriksaan ini dilakukan untuk mencari bakteri Mycobacterium leprae, yang selanjutnya akan digunakan untuk menentukan klasifikasi kusta.
Selain itu, dokter juga dapat melakukan pemeriksaan lepromin. Pada pemeriksaan ini, bakteri yang tidak aktif akan disuntikkan sedikit ke bawah kulit. Selanjutnya, dokter akan mengamati bagian yang disuntikkan setelah 3 hari dan 28 hari, untuk melihat reaksi kekebalan tubuh. Ada tidaknya reaksi akan membantu dokter dalam menentukan klasifikasi kusta berdasarkan kriteria Ridley-Jopling. Orang yang tidak menderita kusta tidak akan memiliki reaksi apapun terhadap tes ini.
Tata Laksana
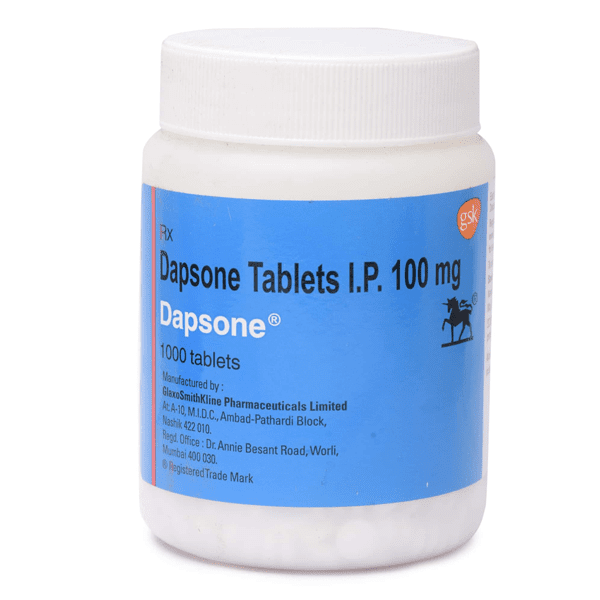
Terapi standar untuk kusta adalah antibiotik kombinasi dosis tetap (KDT). Antibiotik ini diberikan bersamaan untuk mencegah kekebalan bakteri terhadap obat (resistensi obat). Obat-obatan yang biasa digunakan adalah dapson, rifampin, dan klofazimin. Dosis obat-obatan ini berbeda tergantung klasifikasi kusta. Tidak hanya itu, obat-obatan ini diberikan dalam waktu yang lama, berkisar antara 12 bulan sampai 24 bulan.
Tata laksana juga dilakukan untuk menangani reaksi kusta. Biasanya, dokter akan memberikan obat-obatan untuk menurunkan peradangan pada tubuh akibat reaksi tersebut.
Komplikasi
Penyakit kusta memiliki komplikasi yang cukup parah jika tidak segera ditangani. Komplikasi tersebut berupa:
- Perubahan bentuk anggota gerak tubuh
- Rambut rontok, terutama pada alis dan bulu mata
- Kelemahan otot
- Kerusakan saraf permanen pada tangan dan kaki
- Ketidakmampuan menggunakan tangan dan kaki
- Hidung tersumbat kronik, mimisan, dan runtuhnya batas antara lubang hidung kanan dan kiri
- Peradangan selaput pelangi pada mata
- Glaukoma, penyakit mata yang menyebabkan kerusakan pada saraf mata
- Kebutaan
- Masalah ereksi pada pria
- Kemandulan
- Gagal ginjal
Pencegahan
Cara terbaik untuk mencegah kusta adalah menghindari kontak erat jangka panjang dengan penderita kusta yang belum ditangani.
Kapan harus ke dokter?
Jika Anda memiliki luka pada kulit yang diikuti mati rasa atau tiba-tiba mati rasa pada anggota gerak tubuh, Anda dapat berkonsultasi dengan dokter. Semakin cepat kusta terdiagnosis, semakin cepat pula penanganan akan dilakukan sebelum penyakit menyebar ke bagian tubuh lainnya dan semakin parah. Kusta merupakan penyakit yang sulit terdiagnosis dengan cepat karena penampakannya yang mirip dengan berbagai penyakit lainnya, sehingga disebut sebagai “the great imitator” (peniru ulung). Anda mungkin perlu untuk mengamati gejala penyakit Anda dan kontrol ke dokter beberapa kali sebelum terdiagnosis kusta.
Mau tahu informasi seputar penyakit lainnya? Cek di sini, ya!
- dr Nadia Opmalina
Bhandari, J., Awais, M., Robbins, B., & Gupta, V. (2021). Leprosy. Retrieved 11 May 2022, from https://www.ncbi.nlm.nih.gov/books/NBK559307/
Donohue, M., & Sampson, S. (2022). Leprosy: Symptoms, Pictures, Types, and Treatment. Retrieved 11 May 2022, from https://www.healthline.com/health/leprosy
Leprosy. (2022). Retrieved 11 May 2022, from https://www.who.int/news-room/fact-sheets/detail/leprosy
Miller, K., & Nazario, B. (2020). Leprosy Symptoms, Treatments, History, and Causes. Retrieved 11 May 2022, from https://www.webmd.com/skin-problems-and-treatments/guide/leprosy-symptoms-treatments-history