Definisi
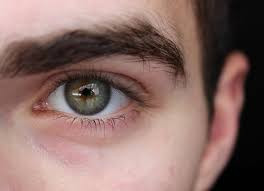
Iritis adalah peradangan pada iris, yaitu lingkaran berwarna yang mengelilingi pupil (lingkaran hitam di tengah mata). Iris merupakan bagian yang memberi warna pada mata karena mengandung pigmen. Selain berfungsi memberi warna, iris juga bertugas mengontrol banyaknya cahaya yang masuk melalui pupil lewat kerja serabut otot yang dimilikinya. Hal inilah yang membuat pupil akan mengecil ketika cahaya terang dan melebar pada cahaya redup. Penyebab iritis seringkali tidak diketahui, namun faktor genetik terbukti berperan terhadap munculnya iritis.
Penyebab
Seringkali, penyebab iritis tidak diketahui. Dalam beberapa kasus, iritis berkaitan dengan cedera mata, faktor genetik, atau penyakit tertentu, terutama penyakit autoimun. Penyebab iritis antara lain:
- Cedera mata. Luka karena benda tumpul, luka tajam, maupun luka bakar karena bahan kimia atau api dapat menyebabkan iritis akut (baru terjadi).
- Infeksi. Infeksi virus pada wajah juga dapat menyebabkan iritis. Infeksi kuman pada bagian tubuh lain juga berhubungan dengan iritis, seperti tuberkulosis (infeksi bakteri Mycobacterium tuberculosis), sifilis (infeksi menular seksual oleh bakteri Treponema pallidum), atau toksoplasmosis (infeksi parasit Toxoplasma gondii).
- Faktor genetik. Orang dengan penyakit autoimun (penyakit yang menyerang sistem kekebalan tubuh) tertentu karena mutasi gen, dapat mengalami iritis akut. Penyakit autoimun tersebut antara lain artritis (radang sendi) psoriatik, spondilitis ankilosa (radang sendi pada tulang belakang), dan inflammatory bowel disease (radang usus).
- Penyakit Behcet. Penyakit ini merupakan penyebab iritis akut yang jarang terjadi, kondisi ini ditandai dengan masalah persendian, sariawan, dan luka pada area genital.
- Juvenile rheumatoid arthritis (rematik pada remaja). Iritis kronis dapat berkembang pada anak-anak dengan kondisi ini.
- Sarkoidosis, yaitu peradangan yang mengenai berbagai bagian tubuh, seperti paru-paru, kelenjar getah bening, mata, dan kulit. Penyakit autoimun ini dapat menyebabkan munculnya kumpulan sel inflamasi di area tubuh, termasuk mata.
- Penyakit Kawasaki, yaitu peradangan dinding pembuluh darah.
- Kolitis ulseratif, yaitu peradangan usus besar.
- Obat-obatan tertentu. Beberapa obat, seperti antibiotik Rifabutin dan obat antivirus Cidofovir yang digunakan untuk mengobati infeksi HIV dapat menjadi penyebab iritis yang jarang terjadi. Bifosfonat, yang merupakan obat osteoporosis, juga dapat menyebabkan iritis. Dengan menghentikan penggunaan obat-obatan tersebut, akan menghentikan gejala iritis yang timbul.
Faktor Risiko
Risiko Anda terkena iritis meningkat jika Anda:
- Memiliki mutasi gen tertentu. Orang dengan mutasi pada gen yang berperan penting dalam sistem kekebalan tubuh berpeluang lebih besar mengalami iritis.
- Mengalami infeksi menular seksual. Infeksi tertentu seperti sifilis atau HIV/AIDS, berkaitan dengan risiko iritis.
- Memiliki sistem kekebalan yang lemah atau gangguan pada sistem kekebalan tubuh. Hal ini termasuk pada penyakit spondilitis ankilosa dan artritis
- Merokok. Penelitian membuktikan bahwa rokok dapat meningkatkan risiko Anda mengalami iritis.
Gejala
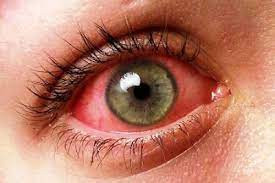
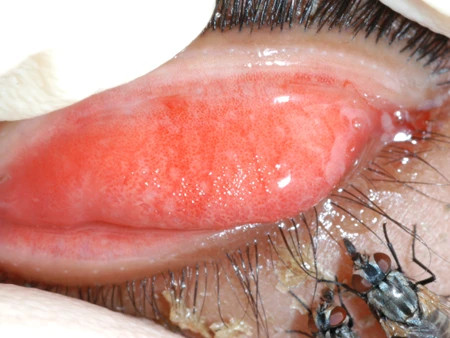
Iritis dapat terjadi pada satu atau kedua mata. Biasanya muncul tiba-tiba dan dapat menetap hingga tiga bulan. Tanda dan gejala iritis antara lain:
- Mata merah
- Rasa nyeri atau tidak nyaman pada mata
- Nyeri kepala, terutama sekitar mata
- Sensitif terhadap cahaya
- Bentul pupil terlihat tidak beraturan
- Penurunan penglihatan jika sudah kronik (berlangsung lama)
Iritis yang baru muncul dalam beberapa hari, disebut iritis akut. Sedangkan yang menetap lebih dari tiga bulan disebut iritis kronik.
Diagnosis
Untuk mendiagnosis iritis, dokter mata akan melakukan wawancara dan pemeriksaan mata lengkap. Wawancara berisi pertanyaan mengenai tanda dan gejala yang dirasakan dan riwayat penyakit lainnya. Setelah itu, dokter akan melakukan beberapa pemeriksaan mata berikut:
- Pemeriksaan luar. Dokter melakukan pemeriksaan menggunakan senter untuk melihat pupil, mengamati pola kemerahan pada mata, dan memeriksa apakah ada cairan atau kotoran mata yang berlebih.
- Pemeriksaan ketajaman penglihatan. Dokter akan menguji ketajaman penglihatan Anda menggunakan grafik khusus dan tes standar lainnya.
- Pemeriksaan slit lamp. Dokter akan melihat bagian dalam mata Anda dan mencari tanda-tanda iritis menggunakan mikroskop khusus. Dengan melebarkan pupil Anda menggunakan obat tetes mata khusus, dokter dapat melihat bagian dalam mata Anda dengan lebih baik
Jika dokter mata mencurigai ada suatu penyakit atau kondisi yang menyebabkan iritis, dokter akan bekerja sama dengan dokter ahli lainnya untuk menentukan penyebab iritis Anda. Dalam hal ini, mungkin diperlukan pemeriksaan lebih lanjut seperti tes darah atau foto X-ray untuk menemukan atau menyingkirkan penyebab iritis.
Tata Laksana
Pengobatan iritis bertujuan untuk mempertahankan penglihatan serta menghilangkan rasa sakit dan peradangan. Untuk iritis yang terkait dengan penyakit lain, mengobati penyakit tersebut akan membantu penyembuhan.
Obat yang biasa diresepkan oleh dokter mata antara lain obat tetes mata antiradang dan pelebar pupil untuk mengurangi rasa nyeri. Obat pelebar pupil juga melindungi mata dari komplikasi yang dapat mengganggu fungsi pupil. Jika gejala tidak mereda atau tampak memburuk, dokter dapat meresepkan obat-obatan minum yang sesuai dengan kondisi Anda. Jika kondisi mata serius atau muncul komplikasi, operasi dapat menjadi pilihan lain dalam pengobatan.
Setelah mendapat pengobatan dari dokter mata, berikut beberapa langkah yang dapat Anda lakukan untuk perawatan di rumah:
- Mengikuti aturan penggunaan obat sesuai arahan dokter
- Menggunakan kacamata gelap jika cahaya membuat mata Anda terasa sakit
- Anda dapat mengkonsumsi obat antinyeri jika diperlukan
Jika iritis disebabkan oleh cedera mata, umumnya akan sembuh dalam waktu 1-2 minggu. Pada kasus lain, mungkin sembuh dalam hitungan minggu hingga bulan.
Komplikasi
Jika tidak diobati dengan benar, iritis dapat menyebabkan beberapa komplikasi berikut:
- Katarak, yaitu kekeruhan pada lensa mata. Komplikasi ini mungkin terjadi, terutama jika peradangan terjadi dalam waktu lama.
- Bentuk pupil tidak beraturan. Jaringan parut yang muncul akibat peradangan dapat menyebabkan iris menempel pada lensa atau kornea, sehingga membuat bentuk pupil tidak beraturan dan iris lambat dalam bereaksi terhadap cahaya.
- Glaukoma, yaitu peningkatan tekanan bola mata dan kerusakan saraf. Komplikasi ini dapat menyebabkan kehilangan penglihatan.
- Penumpukan kalsium pada kornea (band keratopathy). Hal ini menyebabkan kerusakan kornea dan dapat menurunkan penglihatan.
- Pembengkakan pada retina (lapisan belakang mata yang menangkap cahaya). Pembengkakan tersebut dapat menurunkan area penglihatan sentral Anda.
Pencegahan
Pencegahan iritis termasuk sulit dilakukan karena sebagian besar iritis tidak diketahui penyebabnya. Namun, deteksi dini dan penanganan segera dapat mengurangi risiko hilangnya penglihatan yang bersifat permanen. Selain itu, mengobati penyakit lain yang mendasari, seperti penyakit autoimun, dapat mencegah timbulnya iritis.
Kapan Harus ke Dokter?
Konsultasi dengan dokter mata sesegera mungkin jika Anda memiliki gejala iritis. Penanganan segera dapat membantu mencegah komplikasi serius. Jika Anda memiliki sakit mata dan gangguan penglihatan dengan tanda dan gejala lain, Anda mungkin memerlukan perawatan medis segera. Kemungkinan kekambuhan pada iritis cukup besar. Oleh karena itu, jika Anda mengalami keluhan yang serupa dengan gejala saat terkena iritis sebelumnya, segera konsultasikan ke dokter.\
Mau tahu informasi seputar penyakit lainnya? Cek di sini, ya!
- dr Nadia Opmalina
Muchatuta M. (2019). Iritis and Uveitis. Medscape. Retrieved 19 November 2021, from https://emedicine.medscape.com/article/798323-overview
Mayo Clinic. (2019). Iritis. Mayo Clinic. Retrieved 19 November 2021, from https://www.mayoclinic.org/diseases-conditions/iritis/symptoms-causes/syc-20354961
WebMD. (2020). Iritis. WebMD. Retrieved 19 November 2021, from https://www.webmd.com/eye-health/default.htm